The National Health Service (NHS) in the UK is grappling with a severe winter crisis, exacerbated by a confluence of factors including a surge in respiratory illnesses, bed shortages, and long-standing systemic challenges. A new NHS guideline on managing patient care in hospital corridors, intended to address overcrowding, has sparked controversy among medical professionals. The Royal College of Emergency Medicine (RCEM) has vehemently criticized the guidance, arguing that it normalizes a dangerous practice and fails to address the root causes of the crisis.
The new guidance, released in September, acknowledges the increasing reliance on “temporary escalation spaces,” euphemistically referring to corridors, due to persistent pressure on hospital resources. While the document states that corridor care is “not acceptable” and should not be considered standard practice, it also outlines procedures for providing “safe and good quality care” in these spaces. The RCEM contends that delivering adequate care in corridors is impossible, citing issues such as compromised patient dignity and confidentiality, difficulties in monitoring patients and administering treatment, increased infection risk, and the disruption of rest and sleep. The College emphasizes that overcrowding, leading to extended stays in emergency departments, is the primary driver of this issue and contributes to avoidable patient deaths. They urge the NHS to focus on preventing overcrowding rather than adapting to it.
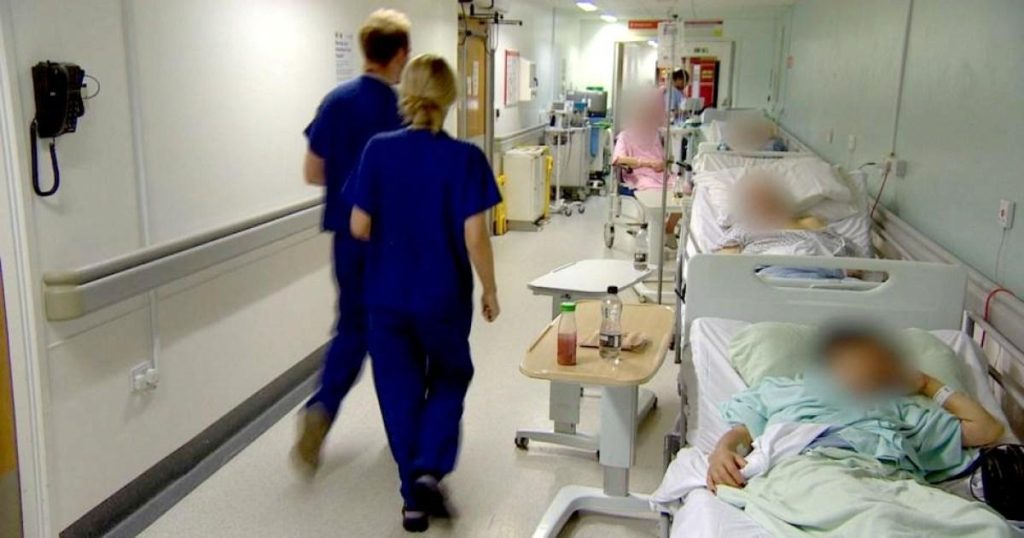
The current winter season presents a particularly acute challenge for the NHS, with a surge in cases of flu, RSV, norovirus, and COVID-19, collectively referred to as the “quad-demic.” This influx of patients, coupled with existing capacity constraints, has led to widespread overcrowding in hospitals, forcing medical staff to resort to using corridors for patient care. First-hand accounts from witnesses describe patients being treated in full view of others, a stark illustration of the compromised dignity and privacy resulting from this practice. Senior midwife Donna Ockenden, who has conducted reviews of patient safety within the NHS, noted that corridor care has become normalized, evidenced by laminated signs designating trolley spaces in hospital corridors.
The normalization of corridor care reflects a deeper systemic issue within the NHS. Years of austerity measures under the previous Conservative government have resulted in funding cuts and resource constraints, impacting the health service’s ability to cope with increasing demand. While the current Labour government has pledged increased funding for the NHS, experts caution that it may not be sufficient to address the underlying problems and alleviate the pressure on hospitals. Data reveals a tenfold increase in wait times exceeding 24 hours for a hospital bed since 2019, further highlighting the strain on the system. Hospitals in England are consistently operating near maximum capacity, with bed occupancy rates exceeding 94% in recent weeks.
The RCEM’s criticism of the new corridor care guidance underscores the urgent need for a systemic overhaul of the NHS to address the root causes of overcrowding. They argue that focusing on managing the consequences of overcrowding rather than tackling the underlying issues is a short-sighted approach that jeopardizes patient safety and well-being. The College calls for a comprehensive strategy to address the underlying capacity constraints, including increased investment in healthcare infrastructure, improved patient flow management, and a greater emphasis on preventative care. This, they argue, is the only way to ensure that patients receive the safe, dignified, and effective care they deserve.
The situation underscores the precarious state of the NHS and the urgent need for action. The debate over the corridor care guidance reflects a broader discussion about the future of the NHS and the challenges it faces in providing quality care amidst increasing demand and limited resources. The government’s response to this crisis will be crucial in determining the long-term health and well-being of the population. While increased funding is a welcome step, it must be accompanied by comprehensive reforms to address the systemic issues plaguing the NHS and ensure its sustainability for future generations.