Alzheimer’s disease, the most prevalent form of dementia, affects millions worldwide, progressively eroding cognitive function and diminishing quality of life. While the exact mechanisms driving this devastating disease remain elusive, recent research has illuminated a critical cellular process that may hold the key to unlocking effective treatments. A team of scientists at the Advanced Science Research Center at The City University of New York (CUNY ASRC) has identified a specific type of microglia, the brain’s primary immune cells, that plays a central role in Alzheimer’s progression. This groundbreaking discovery, published in the journal Neuron, offers a promising new target for drug development aimed at slowing or even reversing the disease’s course.
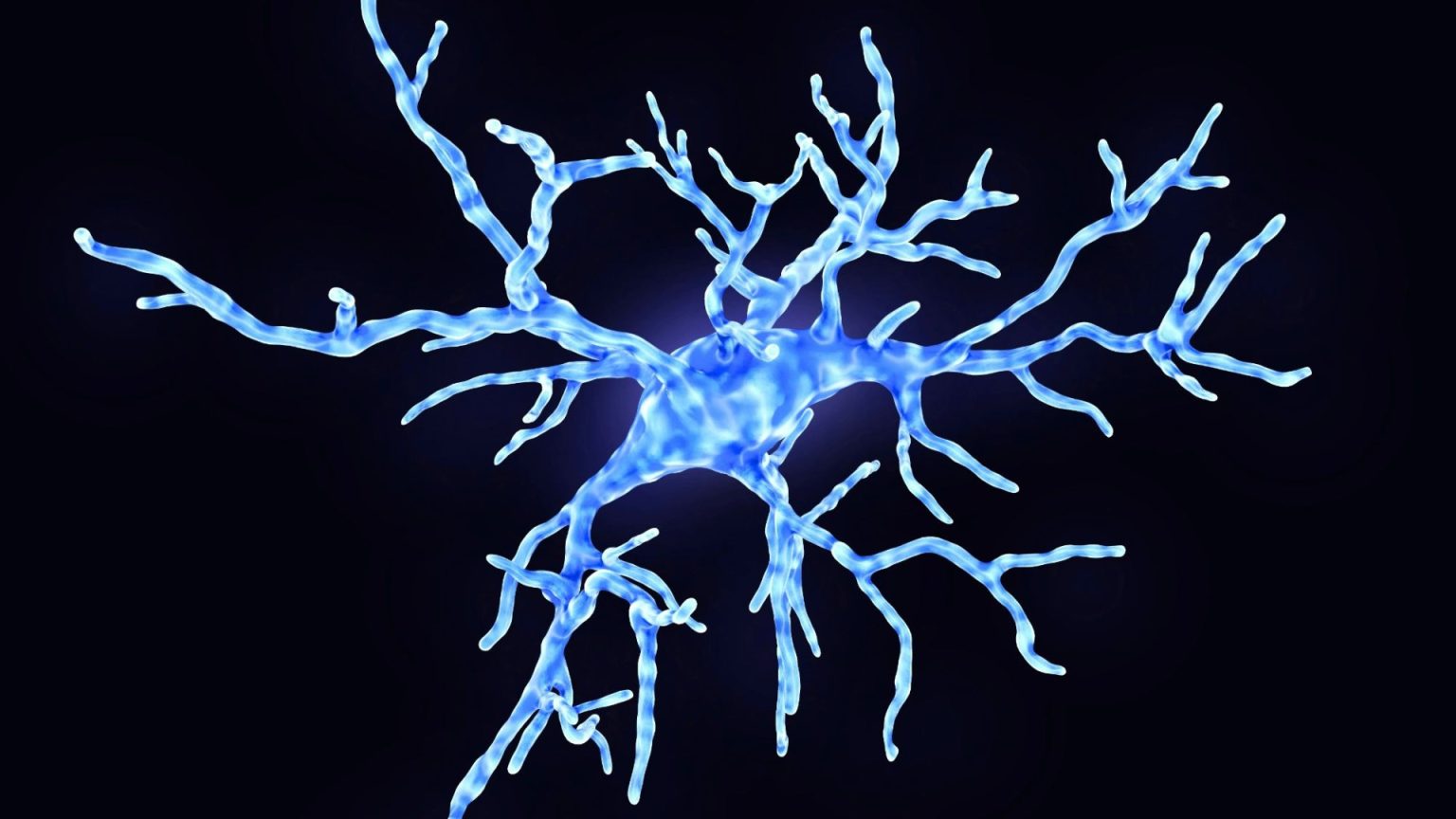
Microglia, often referred to as the brain’s “first responders,” are tasked with protecting the brain from various threats, including infections and injury. However, these cells can exhibit a dual nature, with some subpopulations promoting brain health while others contribute to neurodegeneration. Understanding the intricate balance between these opposing functions has been a primary focus of Professor Pinar Ayata and her team at CUNY ASRC. Their research has pinpointed a specific microglial phenotype, characterized by a stress-related signaling pathway known as the integrated stress response (ISR), that plays a detrimental role in Alzheimer’s disease.
The activation of the ISR pathway in these microglia triggers the production and release of toxic lipids, which damage neurons and oligodendrocyte progenitor cells, two essential cell types crucial for brain function and particularly vulnerable in Alzheimer’s. This finding provides a direct link between cellular stress and the neurotoxic effects of microglia in the disease. Encouragingly, the researchers demonstrated that blocking the ISR pathway or the formation of these toxic lipids could reverse Alzheimer’s-like symptoms in preclinical mouse models, offering a potential therapeutic strategy for human patients.
To further validate their findings, the team examined postmortem brain tissue from Alzheimer’s patients using electron microscopy, a powerful imaging technique that allows for detailed visualization of cellular structures. They observed a significant accumulation of “dark microglia,” a subset of microglia associated with cellular stress and neurodegeneration, in the brain tissue of Alzheimer’s patients. These dark microglia were found at levels twice as high in Alzheimer’s patients compared to healthy individuals, further solidifying the link between these stress-activated microglia and disease progression.
The identification of this specific microglial phenotype and its associated stress pathway represents a significant advance in Alzheimer’s research. By targeting this pathway, researchers hope to develop new drugs that can either halt the production of toxic lipids or prevent the activation of these harmful microglia. This targeted approach holds the potential to significantly slow or even reverse the progression of Alzheimer’s disease, offering hope to millions of individuals and their families affected by this devastating condition.
While these findings represent a promising step forward, further research is needed to translate these preclinical discoveries into effective therapies for human patients. Clinical trials will be essential to evaluate the safety and efficacy of drugs targeting this pathway in humans. However, this groundbreaking research provides a critical piece of the Alzheimer’s puzzle and opens up exciting new avenues for drug development, offering renewed hope for a future where this devastating disease can be effectively treated and perhaps even prevented.