The Care Quality Commission (CQC), the independent regulator of health and social care services in England, has published its latest ratings of GP practices across the country, revealing a mixed picture of performance. While the vast majority of practices are rated as “Good,” a significant number are falling short of expected standards, raising concerns about patient safety and the quality of care.
The CQC’s findings, analyzed by medical negligence specialists Patient Claim Line, show that approximately 5% of GP practices in England, totaling 292, are currently rated as either “Inadequate” or “Requires Improvement.” These subpar ratings indicate a range of issues, including inadequate safety protocols, insufficient staff training, ineffective governance, and a failure to adequately manage health risks. Specific examples highlighted include failures to properly store vaccines, misdiagnosis of serious conditions like diabetes, and inadequate monitoring of patients prescribed high-risk medications. These deficiencies pose a serious threat to patient well-being and underscore the urgent need for improvement in these underperforming practices. Patient Claim Line’s solicitor, Nermeen Salahuddin, emphasized the alarming nature of these shortcomings and called for immediate action to rectify these issues and ensure patient safety.
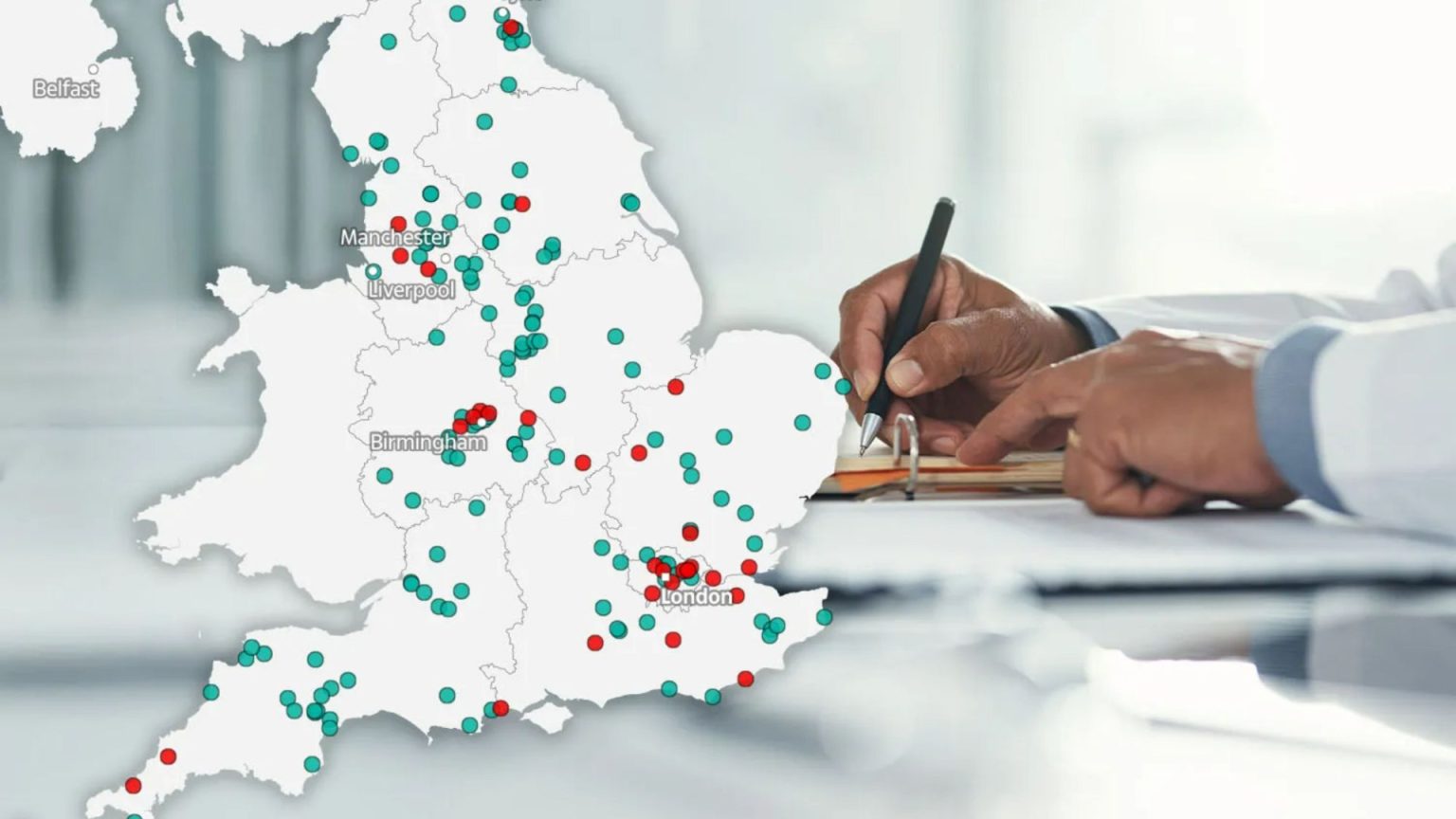
On the other end of the spectrum, the CQC highlighted 278 GP practices, representing about 4.8% of the total, that have achieved an “Outstanding” rating. These practices demonstrate exceptional performance in delivering high-quality care and meeting patient needs. Geographically, these top-performing practices are distributed across the country, with notable concentrations in Devon, Greater Manchester, Nottinghamshire, Derbyshire, the West Midlands, and Cumbria. This positive performance showcases best practices and provides examples for other surgeries to emulate. The vast majority of GP practices, approximately 90% or 5,193 surgeries, received a “Good” rating, indicating that they are generally meeting expectations and providing satisfactory care.
The CQC assesses GP practices based on five key domains: safety, effectiveness, caring, responsiveness, and well-led. These domains provide a comprehensive framework for evaluating the overall quality of care provided by a practice. However, the CQC’s one-word rating system has drawn criticism from some GPs who argue that it is overly simplistic and fails to capture the complexities of primary care. They advocate for a more nuanced approach to evaluation and have even called for the abolition of the current inspection regime. Conversely, others defend the CQC’s methodology, asserting that its inspections and ratings provide a valuable mechanism for ensuring accountability and driving improvements in the healthcare system.
A closer look at the worst-performing practices reveals recurring themes related to patient safety, staffing levels, staff training, governance, and hygiene standards. Examples of specific failings identified by CQC inspectors include inadequate risk management systems, improper storage of vaccines, and failure to maintain appropriate hygiene standards. In some instances, serious clinical errors, such as misdiagnosis of diabetes, have been documented, further highlighting the potential for patient harm. These cases underscore the critical importance of robust systems and processes to safeguard patient well-being.
In contrast, the “Outstanding” rated practices demonstrate excellence across the five key domains assessed by the CQC. These practices prioritize patient safety, provide effective and evidence-based care, demonstrate compassion and empathy towards their patients, are responsive to patient needs and preferences, and are led by strong and effective leadership teams. They serve as exemplars of high-quality primary care and provide valuable lessons for other practices striving to improve their performance.
The CQC’s findings come at a time when the NHS is facing significant challenges, including increasing demand, workforce shortages, and financial constraints. These pressures have led to concerns about the ability of GP practices to provide timely and effective care to their patients. The CQC’s report highlights the importance of addressing the underlying issues contributing to poor performance in some practices and ensuring that all patients have access to safe and high-quality primary care. Initiatives such as “Pharmacy First,” which allows pharmacists to treat seven common ailments, aim to alleviate some of the pressure on GP practices by providing alternative avenues for patients to access care for minor conditions.
The government has also announced plans to increase scrutiny of hospital performance, with Health Secretary Wes Streeting proposing a national league table to rank hospitals based on waiting times, patient care, and financial management. This move reflects a broader effort to improve transparency and accountability within the NHS and to drive improvements in performance across the healthcare system. The aim is to ensure that all NHS providers are meeting the required standards and delivering the best possible care to patients. The varying performance levels highlighted by the CQC’s report underscore the need for ongoing efforts to improve the quality and consistency of care provided by GP practices and across the wider NHS.