A groundbreaking study suggests that a common herpes virus, cytomegalovirus (HCMV), may be implicated in a significant proportion of Alzheimer’s cases. Researchers at Arizona State University have discovered evidence linking HCMV to the development of Alzheimer’s disease in up to 45% of individuals. This specific herpes virus, distinct from those causing cold sores or sexually transmitted infections, is typically contracted during childhood and often remains dormant without causing noticeable symptoms. However, the research team posits that in certain individuals, HCMV can reactivate and travel from the gut to the brain via the vagus nerve, a crucial pathway connecting the two organs.
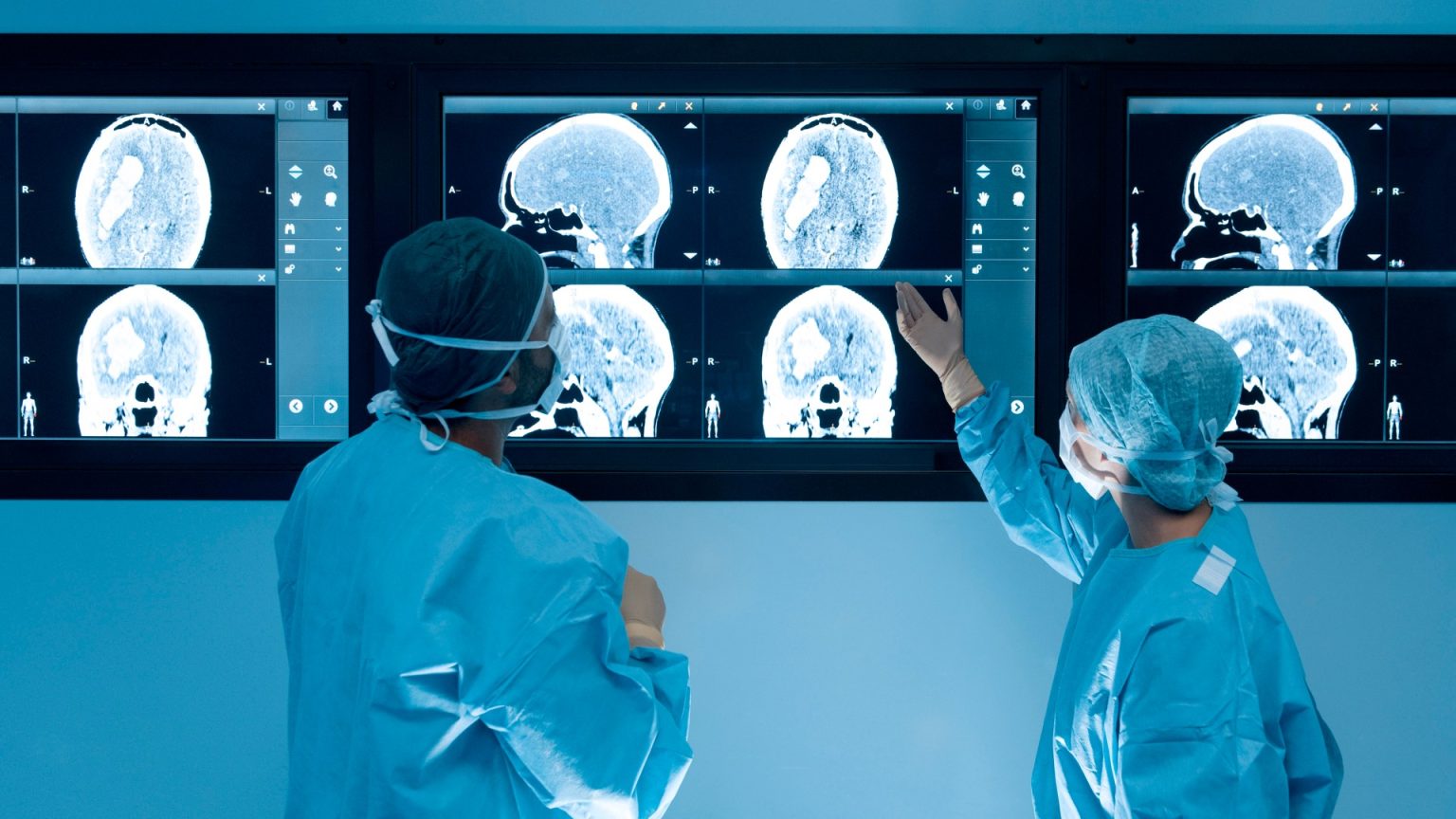
Once in the brain, HCMV appears to trigger immune responses that contribute to the formation of amyloid plaques and tau tangles, hallmarks of Alzheimer’s disease. These abnormal protein accumulations disrupt communication between brain cells, leading to the cognitive decline characteristic of the disease. The researchers identified a distinct subtype of Alzheimer’s characterized not only by the typical amyloid plaques and tau tangles but also by a unique viral footprint, including specific antibodies and immune cells indicative of inflammation. Post-mortem examinations of Alzheimer’s patients revealed increased levels of inflammation-driving immune cells, alongside evidence of viral activity in the gut and spinal fluid. Furthermore, traces of the virus were found in the vagus nerve, supporting the hypothesis that this nerve serves as a conduit for the virus to reach the brain.
While HCMV is widespread, with approximately 80% of individuals carrying antibodies by age 80, the researchers observed active HCMV infections specifically in individuals with Alzheimer’s, solidifying the potential link between the virus and the disease. This discovery offers a new perspective on the development of Alzheimer’s, suggesting that a readily treatable viral infection could be a key contributing factor in a substantial portion of cases. The research team is actively developing a blood test to detect active HCMV infections, paving the way for early intervention and potentially preventing the onset of Alzheimer’s.
The implications of this research are far-reaching, potentially revolutionizing the diagnosis, treatment, and prevention of Alzheimer’s disease. Existing antiviral medications could be repurposed to treat or prevent this HCMV-related subtype of Alzheimer’s, offering a promising avenue for intervention. The development of a blood test to identify individuals with active HCMV infections would enable targeted treatment with antivirals, potentially halting the progression of the disease or even preventing its onset altogether.
This study underscores the complex interplay between viral infections and neurodegenerative diseases. While further research is needed to confirm these findings and explore the precise mechanisms by which HCMV contributes to Alzheimer’s development, this discovery opens up exciting new possibilities for tackling this devastating disease. The potential for using existing antiviral drugs to treat or prevent this form of Alzheimer’s represents a significant step forward in the fight against this debilitating condition. The development of a blood test for early detection further enhances the potential for effective intervention and prevention strategies.
The findings of this study offer a glimmer of hope in the ongoing battle against Alzheimer’s disease. While current treatments primarily focus on managing symptoms, the potential to target an underlying viral cause offers a paradigm shift in the approach to Alzheimer’s. The development of a readily available blood test for early detection of active HCMV infections could enable timely intervention with antiviral therapies, potentially delaying or even preventing the onset of Alzheimer’s in a significant number of individuals. This breakthrough research highlights the importance of further investigation into the role of viral infections in neurodegenerative diseases and underscores the potential for developing targeted therapies to combat these debilitating conditions.